Decompression Sickness
Decompression sickness (DCS; also known as divers' disease, the bends ) describes a condition arising from dissolved gases coming out of solution into bubbles inside the body on depressurisation.
Decompression sickness occurs in the body after scuba diving because of gases in the body releasing as bubbles on depressurisation. When we are living on dry land at sea level, the air around us has a pressure of 14.7 PSI (pounds per square inch), or one atmosphere. That is a “normal pressure” for our bodies.
Water is heavy compared to air, it does not take much water to exert a lot of pressure. One-inch by one-inch column of water 33 feet high exerts another 14.7 pounds per square inch than the same column of air.
If you hold your breath and dive down 33 feet, your lungs contract in size by a factor of two because there is twice as much pressure around the air in your lungs, making them contract. When you rise back up, the air expands again and your lungs return to normal size.
When you breathe from a scuba tank however, the air coming out of the tank has to have the same pressure as the pressure that the water is exerting. Therefore, when scuba diving, the air in your lungs at a 33-foot depth has twice the pressure of air on land and the pressure continues to double as the depth gets deeper.
Imagine a carbonated drink, Carbonation in liquid is made through high-pressure gases in the air coming in contact with water and dissolving. When you release the pressure in a bottle of carbonated liquid, the dissolved gas quickly rises as bubbles.
If a diver stays under a low depth of water for a certain period of time when diving, some amount of nitrogen from the air will dissolve inside them, much like the gas in carbonated drinks. If they swim to the surface quickly, the dissolves gasses inside their body will react in much the same way as those inside a carbonated drink and come to surface in bubbles.
This occurrence in a human body is called decompression sickness and can cause many problems, at very worst it can be fatal to a diver.
What to do when you have DCS
A doctor should always be called for in the case of the DCS, however there are a few things you can do yourself to treat the symptoms of the DCS, until medical help arrives.
Dry the diver and warm with blankets if their body temperature shows sings of dropping. Administer fluids to fight off dehydration, but do not give aspirin as it may mask symptoms. If you have access to oxygen, a mask should be applied to the diver as soon as possible.
Call both the emergency services and the Divers Alert Network to locate the nearest hyperbaric chamber (100% oxygen delivered in a high-pressure chamber) and to get specialist advice.
The diver will need to lie in a horizontal position when transported and in the case of air transport, the cabin must stay below 1,000 feet, or pressurized to sea level pressure. Use high-flow oxygen throughout transportation and up to the point where a hyperbaric chamber is available.
The duration of treatment depends on the symptoms, the diver’s history and the type of recompression therapy on hand.
Onset of Decompression Sickness
Although onset of DCS can occur rapidly after a dive, in more than half of all cases symptoms do not begin to appear for at least an hour. In extreme cases, symptoms may occur before the dive has been completed. The U.S. Navy and Technical Diving International, a leading technical diver training organization, have published a table that documents time to onset of first symptoms. The table does not differentiate between types of DCS, or types of symptom.
Onset of symptoms
| Time to onset |
|
Percentage of cases |
|
within 1 hour |
|
42% |
|
within 3 hours |
|
60% |
|
within 8 hours |
|
83% |
|
within 24 hours |
|
98% |
|
within 48 hours |
|
100% |
|
|
Most common symptoms
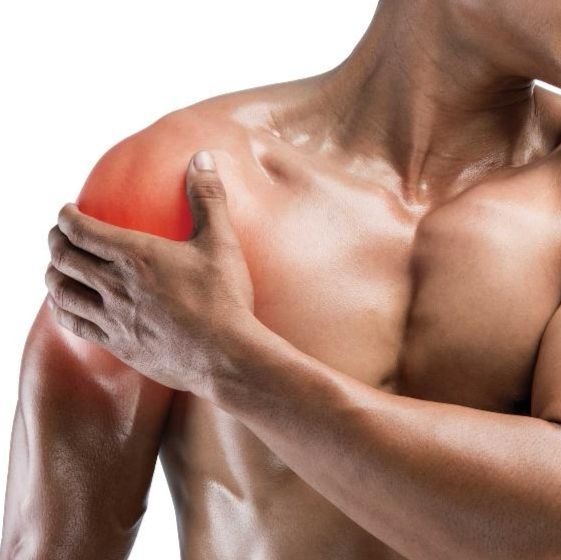
Musculoskeletal Mostly large joints
(elbows, shoulders, hip, wrists, knees, ankles)
Localized deep pain, ranging from mild to excruciating. Sometimes a dull ache, but rarely a sharp pain.
Active and passive motion of the joint aggravates the pain.
The pain may be reduced by bending the joint to find a more comfortable position.
If caused by altitude, pain can occur immediately or up to many hours later.
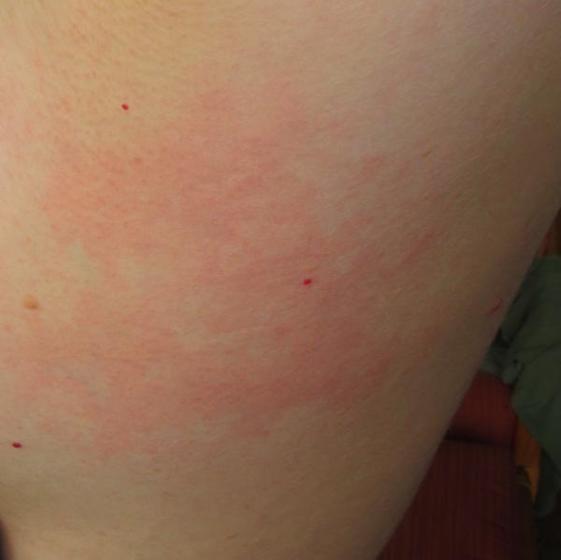
Cutaneous- Skin
Type 1 DCS is usually characterized by musculoskeletal pain and mild cutaneous, or skin, symptoms. Common Type 1 skin manifestations include itching and mild rashes (as distinct from a clear mottled or marbled and sometimes raised discoloration of the skin — a condition that is known as cutis marmorata that may presage the development of the more serious symptoms of Type 2 DCS). Less common but still associated with Type 1 DCS is obstruction of the lymphatic system, which can result in swelling and localized pain in the tissues surrounding the lymph nodes — such as in the armpits, groin or behind the ears.
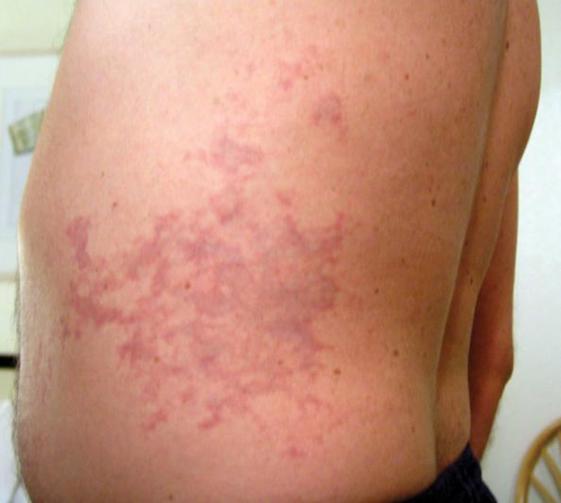
Cutis Marmorata - Marbled skin
Skin mottling like this is characteristic of cutis marmorata, a condition that can warn of likely development of more serious Type 2 symptoms. Past experience in diving medicine has shown that patients initially presented with only this symptom have a high likelihood of progression to neurological, Type II, DCS without prompt treatment. The marbling does not resolve until few days after treatment, but any pruritus (itching) will likely disappear upon initial recompression.

Neurologic-Brain
Altered sensation, tingling or numbness (paresthesia), increased sensitivity (hyperesthesia)
Confusion or memory loss (amnesia)
Visual abnormalities
Unexplained mood or behaviour changes
Seizures, unconsciousness
Neurologic-Spinal cord
Ascending weakness or paralysis in the legs
Urinary incontinence and fecal incontinence
Girdling (also referred to as girdle, banding, or tightening feeling) around the abdominal region and/or chest

Constitutional- Whole body
Headache
Unexplained fatigue
Generalised malaise, poorly localised aches

Audiovestibular- Inner ear
Loss of balance
Dizziness, vertigo, nausea, vomiting
Hearing loss
Pulmonary- Lungs
Dry persistent cough
Burning chest pain under the sternum, aggravated by breathing
Shortness of breath



 Welcome to
Welcome to